Understanding Interstitial Cystitis: A Chronic Bladder Condition
Interstitial cystitis is a long-term condition that affects the bladder and surrounding pelvic region, often leading to persistent discomfort and urinary challenges. Unlike a typical urinary tract infection, this condition does not stem from bacteria, which makes it more complex to diagnose and manage. People dealing with interstitial cystitis often experience recurring pain that can interfere with daily routines and overall well-being. The bladder becomes overly sensitive, sending signals to the brain even when it is not full, which contributes to urgency and frequency issues. Over time, this can create a cycle of discomfort and anxiety, especially when symptoms flare unexpectedly. Many individuals struggle with the unpredictability of the condition, making consistent care essential. Understanding how the condition behaves is the first step toward finding effective Treatment for Interstitial Cystitis Fishers and regaining a sense of control.
Recognizing the Symptoms of Interstitial Cystitis
Symptoms of interstitial cystitis can vary widely, but they often share common patterns that affect daily life. One of the most notable signs is persistent pelvic pain or pressure that does not go away easily. Many individuals also experience a constant urge to urinate, even shortly after emptying the bladder. This urgency can occur throughout the day and night, disrupting sleep and productivity. Pain may intensify as the bladder fills and temporarily ease after urination, creating a repetitive and exhausting cycle. Some people also report discomfort during physical activities or intimate moments, adding another layer of difficulty. The severity of symptoms can shift over time, with some days feeling manageable and others significantly more intense. Recognizing these patterns early can help guide appropriate Treatment for Interstitial Cystitis Fishers and prevent symptoms from worsening.
Causes and Risk Factors Behind Interstitial Cystitis
The exact cause of interstitial cystitis remains unclear, but several contributing factors are widely considered by medical professionals. One possible cause is a defect in the bladder lining, which allows irritating substances in urine to penetrate and trigger inflammation. Another theory involves an autoimmune response, where the body mistakenly attacks its own bladder tissue. Nerve hypersensitivity is also believed to play a role, amplifying pain signals beyond normal levels. Chronic inflammation within the bladder can further exacerbate symptoms and make healing more difficult. Women are more commonly affected than men, although the condition can occur in anyone. Age, stress levels, and certain underlying health conditions may also increase the likelihood of developing this disorder. Understanding these risk factors helps guide personalized Treatment for Interstitial Cystitis Fishers that addresses both symptoms and potential triggers.
Why Seeking Treatment for Interstitial Cystitis Fishers Matters
Seeking professional care for interstitial cystitis is essential for improving quality of life and preventing complications. Without proper treatment, symptoms can become more severe and harder to manage over time. Chronic pain and frequent urination can disrupt sleep, work, and social interactions, leading to emotional strain. Many individuals also experience anxiety or frustration due to the unpredictable nature of flare-ups. Accessing Treatment for Interstitial Cystitis Fishers ensures that patients receive targeted care tailored to their specific needs. Local specialists often understand the importance of a comprehensive approach that includes both medical and lifestyle strategies. Early intervention can reduce symptom severity and help individuals maintain a more balanced and active lifestyle. Taking action sooner rather than later can make a significant difference in long-term outcomes.
Diagnostic Process for Interstitial Cystitis
Diagnosing interstitial cystitis involves a thorough evaluation to rule out other conditions with similar symptoms. Healthcare providers typically begin with a detailed review of medical history and symptom patterns. Patients may be asked to track their urination frequency and pain levels over several days. A physical examination, including a pelvic exam, helps identify any abnormalities or areas of tenderness. Laboratory tests such as urinalysis and urine culture are used to eliminate infections as a cause. In some cases, procedures like cystoscopy allow doctors to examine the bladder more closely. Imaging tests may also be recommended to rule out other issues such as kidney stones or tumors. This comprehensive process ensures that the chosen Treatment for Interstitial Cystitis Fishers is accurate and effective.
First-Line Treatments: Lifestyle and Behavioral Modifications
Lifestyle adjustments often serve as the foundation for managing interstitial cystitis symptoms. Dietary changes play a crucial role, as certain foods and beverages can irritate the bladder and trigger flare-ups. Common irritants include caffeine, alcohol, citrus fruits, and spicy foods, which patients are often advised to limit or avoid. Staying properly hydrated is equally important, as it helps dilute urine and reduce irritation. Bladder training techniques can gradually increase the time between urination, improving bladder control. Stress management is another key factor, as emotional tension can intensify symptoms. Practices such as deep breathing, mindfulness, and gentle exercise can help regulate the body’s response to stress. These strategies form an essential part of Treatment for Interstitial Cystitis Fishers, offering a non-invasive way to manage symptoms effectively.
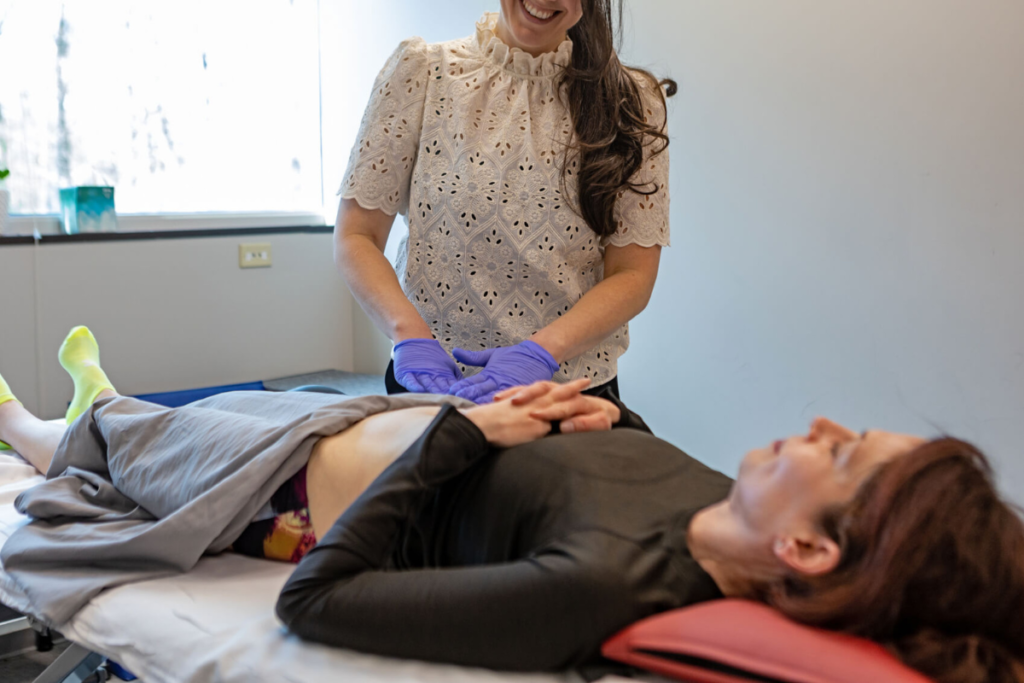
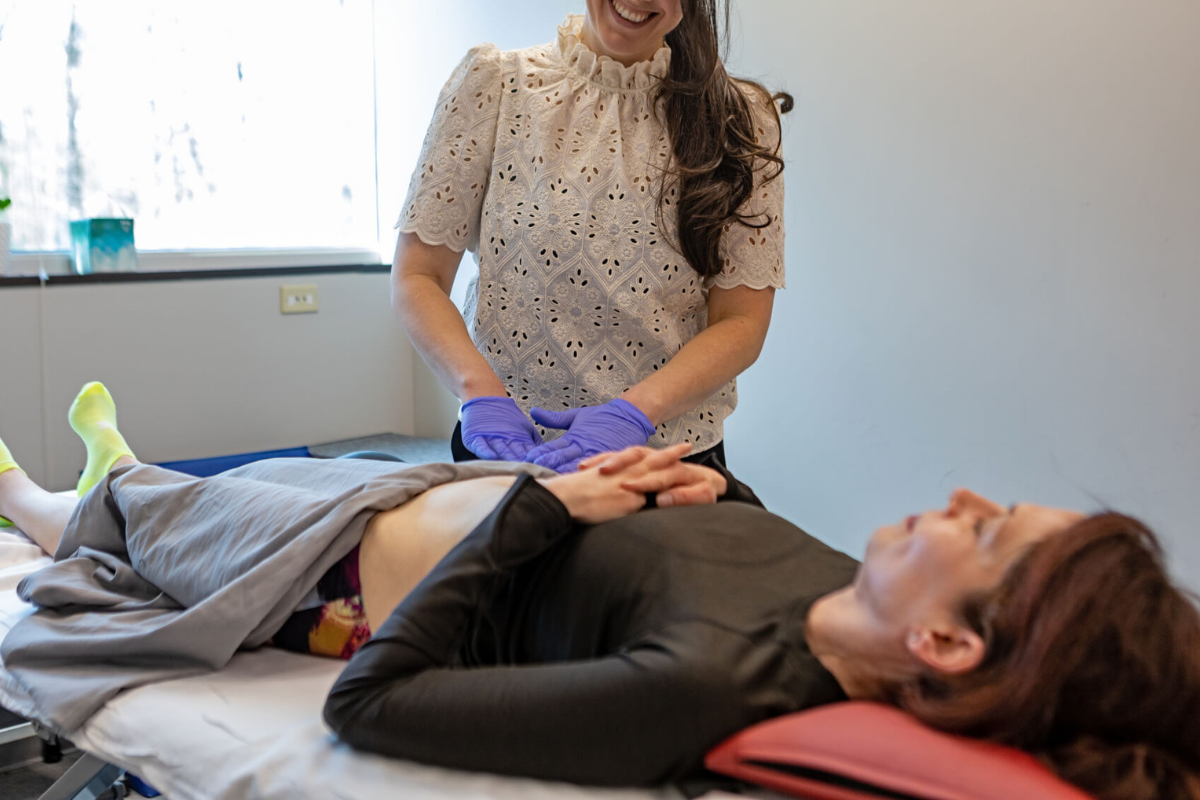
Physical Therapy for Pelvic Floor Dysfunction
Pelvic floor dysfunction is commonly associated with interstitial cystitis, making physical therapy a valuable treatment option. Tight or weakened pelvic muscles can contribute to pain and urinary issues, worsening overall symptoms. Specialized physical therapists use targeted techniques to address these imbalances and improve muscle function. Manual therapy helps release tension and restore proper alignment within the pelvic region. Stretching and strengthening exercises are tailored to each individual’s needs, promoting better control and stability. Biofeedback technology may also be used to help patients become more aware of their muscle activity. Over time, these therapies can significantly reduce pain and improve bladder function. Incorporating physical therapy into Treatment for Interstitial Cystitis Fishers provides a holistic approach that addresses both symptoms and underlying causes.
Medications for Interstitial Cystitis Relief
Medications can play an important role in managing the symptoms of interstitial cystitis, especially for individuals with moderate to severe discomfort. Oral medications such as pain relievers help reduce inflammation and improve daily comfort. Antihistamines may be prescribed to control allergic responses that can contribute to bladder irritation. Tricyclic antidepressants are sometimes used to relax the bladder and reduce pain signals. Bladder instillation therapies involve placing medication directly into the bladder, providing targeted relief. Each medication works differently, so treatment plans are often customized to achieve the best results. Patients may need to try several options before finding the most effective combination. With proper medical guidance, medications can become a key component of Treatment for Interstitial Cystitis Fishers.
Advanced Treatment Options for Persistent Cases
For individuals who do not respond to initial treatments, advanced options may offer additional relief. Nerve stimulation therapies, also known as neuromodulation, help regulate communication between the bladder and the brain. This approach can reduce urgency and frequency by calming overactive nerve signals. Bladder distention procedures temporarily stretch the bladder, which may decrease pain and improve capacity. Botox injections are another option, relaxing the bladder muscles and reducing spasms. In rare cases, surgical interventions may be considered when all other treatments have failed. These procedures are typically reserved for severe cases and require careful evaluation. Exploring advanced Treatment for Interstitial Cystitis Fishers ensures that patients have access to a full range of solutions tailored to their needs.
Integrative and Holistic Approaches
Many individuals find relief by combining traditional medical treatments with holistic approaches. Acupuncture is one option that may help reduce pain and improve overall well-being. Herbal supplements are sometimes used to support bladder health, although they should be taken under professional guidance. Mind-body techniques such as meditation and yoga can help manage stress and promote relaxation. Breathing exercises are particularly useful for calming the nervous system and reducing symptom intensity. These approaches focus on treating the whole person rather than just the condition. When used alongside conventional methods, they can enhance the effectiveness of Treatment for Interstitial Cystitis Fishers. A balanced approach often leads to more sustainable and long-term improvements.
Managing Interstitial Cystitis in Daily Life
Living with interstitial cystitis requires ongoing adjustments to maintain comfort and stability. Planning ahead for work and travel can help reduce stress and avoid unexpected flare-ups. Carrying essentials such as water, medications, and comfort items can make daily routines more manageable. Creating a supportive environment at home and work can also ease the burden of symptoms. Pain management techniques, including heat therapy and relaxation exercises, can provide immediate relief when needed. Building a strong support system with family, friends, or support groups can make a significant difference. Emotional well-being is just as important as physical health when managing a chronic condition. Consistent self-care is a vital part of Treatment for Interstitial Cystitis Fishers.
Choosing the Right Provider for Treatment for Interstitial Cystitis Fishers
Selecting the right healthcare provider is a critical step in managing interstitial cystitis effectively. Patients should look for professionals with experience in pelvic health and chronic bladder conditions. A compassionate approach is equally important, as managing IC often requires ongoing communication and support. Asking detailed questions during consultations can help patients understand their options and feel more confident in their care plan. Personalized treatment strategies are essential, as no two cases are exactly alike. Access to a multidisciplinary team can provide a more comprehensive approach to care. Local providers offering Treatment for Interstitial Cystitis Fishers often combine expertise with convenience, making it easier for patients to stay consistent with their care. Building a strong relationship with a trusted provider can greatly improve long-term outcomes.
Long-Term Care and Monitoring
Managing interstitial cystitis is an ongoing process that requires regular monitoring and adjustments. Symptoms can change over time, making it important to stay proactive in treatment planning. Keeping a symptom journal can help identify patterns and triggers, allowing for more precise management. Regular check-ins with healthcare providers ensure that treatments remain effective and relevant. Preventing flare-ups often involves maintaining healthy habits and avoiding known triggers. Patients are encouraged to stay informed about new therapies and advancements in care. A long-term approach helps maintain stability and reduces the likelihood of severe episodes. Consistent attention to Treatment for Interstitial Cystitis Fishers supports better health and improved quality of life.
Frequently Asked Questions (FAQ)
1. What is the main cause of interstitial cystitis?
The exact cause is not fully understood, but it may involve bladder lining defects, nerve sensitivity, autoimmune responses, or chronic inflammation.
2. Can interstitial cystitis be cured permanently?
There is no permanent cure, but symptoms can be effectively managed with the right combination of treatments and lifestyle changes.
3. What foods should I avoid with IC?
Common triggers include caffeine, alcohol, spicy foods, acidic fruits, and artificial sweeteners.
4. How long does treatment take to show results?
Results vary depending on the individual and treatment type, but some people notice improvements within weeks while others may take longer.
5. Is interstitial cystitis the same as a urinary tract infection?
No, IC is a chronic condition without bacterial infection, while UTIs are caused by bacteria and typically treated with antibiotics.
6. Are there non-medication options available?
Yes, lifestyle changes, pelvic floor therapy, stress management, and dietary adjustments are effective non-medication options.
7. When should I seek professional help?
If you experience persistent bladder pain, urgency, or frequent urination that does not improve, it is important to consult a healthcare provider.
Takeaway
Finding the right path for managing interstitial cystitis requires patience, persistence, and a personalized approach. From lifestyle adjustments and physical therapy to medications and advanced procedures, a wide range of options exists to address different levels of severity. Consistency in care and awareness of triggers can significantly reduce flare-ups and improve daily comfort. Accessing reliable Treatment for Interstitial Cystitis Fishers allows individuals to work closely with experienced providers who understand the complexities of this condition. A balanced combination of medical care and self-management strategies often leads to better long-term outcomes. Staying informed and proactive empowers individuals to take control of their health and maintain a higher quality of life.