Understanding Corneal Transplant
A corneal transplant, or keratoplasty, is a surgical procedure that replaces a damaged or diseased cornea with healthy donor tissue. The cornea is the transparent front layer of the eye, crucial for focusing light and producing clear vision. When the cornea becomes damaged from conditions like scarring, thinning, or disease, vision can deteriorate significantly. Corneal transplantation restores clarity and functionality, often dramatically improving a patient’s quality of life. There are several types of corneal transplants tailored to specific conditions. Full-thickness transplants, known as penetrating keratoplasty, replace the entire cornea. Partial-thickness transplants, such as lamellar or endothelial keratoplasty, replace only the damaged layers, allowing for quicker recovery and fewer complications. Understanding these procedures empowers patients to make informed decisions with their ophthalmologist.
Conditions That Require Corneal Transplant
Corneal transplant is recommended for patients with severe corneal damage that cannot be treated with medications or other procedures. Some of the most common conditions include:
- Keratoconus, a progressive thinning of the cornea causing distorted vision
- Corneal scarring from infections such as bacterial or viral keratitis
- Corneal dystrophies, including Fuchs’ dystrophy, which cause swelling and clouding
- Trauma or chemical burns leading to permanent corneal damage
- Severe swelling or edema after previous eye surgeries
- Failed previous corneal transplants requiring replacement
Early diagnosis and treatment improve the chances of successful vision restoration and prevent further damage. Identifying these conditions in time ensures the patient receives the right type of transplant for their needs.
Preparing for Corneal Transplant Surgery
Successful corneal transplant surgery begins with careful preparation. Patients undergo a complete eye examination, including imaging tests like corneal topography or optical coherence tomography, to assess the extent of damage. Selecting the right donor cornea is crucial, taking into account tissue quality, donor age, and compatibility. Patients are also evaluated for overall health factors, such as diabetes or immune disorders, which could affect healing. Pre-surgery instructions typically include stopping certain medications, avoiding contact lenses, and arranging support for post-operative care. Surgeons also discuss what patients should expect during and after the procedure to reduce anxiety. Proper preparation not only increases the likelihood of surgical success but also shortens recovery time.
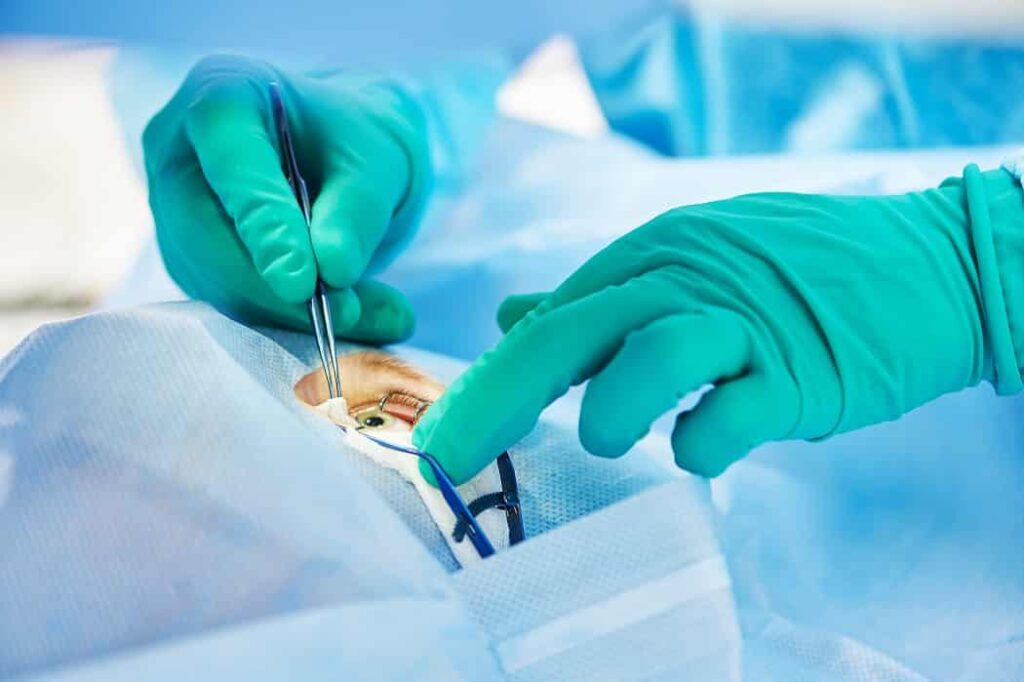
The Corneal Transplant Procedure
Corneal transplant surgery requires precision and careful handling of the donor tissue. The procedure usually begins with local or general anesthesia, depending on the patient’s needs and the type of transplant. The damaged cornea is carefully removed, and the donor cornea is placed in position. Full-thickness transplants replace the entire cornea, while partial-thickness procedures target only the affected layers. Fine sutures or specialized adhesive techniques secure the graft in place. The surgery usually lasts between one and two hours, and most patients can go home the same day or after a short hospital stay. Immediate post-operative care includes protecting the eye, monitoring pressure, and using prescribed medications to prevent infection. Precision during surgery directly impacts graft survival and visual outcomes.
Recovery and Post-Operative Care
Recovery after corneal transplant surgery involves careful monitoring and adherence to medical instructions. Patients may experience blurred vision, sensitivity to light, or mild discomfort, all of which improve gradually. Eye drops are prescribed to reduce inflammation, prevent infection, and promote healing. Protective eyewear may be recommended to avoid accidental trauma during daily activities. Follow-up visits allow ophthalmologists to monitor graft health and detect early signs of rejection. Recovery timelines differ depending on the type of transplant, with partial-thickness procedures generally leading to quicker improvement. Maintaining hygiene, avoiding strenuous activities, and following medication schedules support successful recovery. Long-term care includes protecting the eye, avoiding injuries, and attending routine check-ups to preserve vision.
Risks and Complications
While corneal transplant is highly effective, it carries potential risks. Common complications include infection, swelling, and post-operative astigmatism that may require corrective lenses. Graft rejection is the most serious complication, occurring when the immune system attacks the donor tissue. Signs of rejection include redness, pain, sudden vision changes, or increased sensitivity to light. Prompt treatment, usually with corticosteroids, is critical to saving the graft. Other risks include surgical complications or tissue issues from the donor. Patients can minimize these risks by strictly following post-operative care instructions and reporting any unusual symptoms immediately. Long-term graft survival depends on continued monitoring and healthy eye care practices.
Success Rates and Long-Term Outcomes
Corneal transplants have a high success rate when performed under optimal conditions. Penetrating keratoplasty restores functional vision in approximately 70-90% of cases, while partial-thickness transplants tend to offer faster recovery and lower rejection risk. Factors influencing outcomes include patient health, the underlying condition, age, and adherence to post-surgery care. Visual improvement can continue over months or even years. Patients should maintain regular eye check-ups and avoid eye trauma to ensure long-term graft survival. Proper post-operative care, a healthy lifestyle, and management of systemic conditions contribute to overall success. Advances in surgical techniques and tissue preservation have significantly increased safety and long-term vision outcomes for patients.
Innovations in Corneal Transplantation
Modern corneal transplant techniques have transformed outcomes for patients worldwide. Endothelial keratoplasty, including DMEK and DSEK, replaces only the inner corneal layer, resulting in faster recovery and fewer complications. Artificial corneas, or keratoprostheses, offer solutions for patients ineligible for traditional transplants. Advances in donor tissue preservation extend the usability of corneas, improving accessibility and success rates. Laser-assisted techniques enhance surgical precision, reducing post-operative astigmatism. Stem cell therapy and regenerative medicine are emerging fields that may repair damaged corneal tissue without full-thickness transplants. These innovations highlight the evolving nature of corneal surgery and the potential for even better patient outcomes in the future.
Patient Experiences and Expectations
Understanding what to expect before and after surgery can ease patient anxiety. Immediately after the procedure, blurred vision and light sensitivity are normal and typically improve over time. Emotional reactions, including relief, excitement, or anxiety, are common. Clear guidance on medications, activity restrictions, and warning signs ensures patients remain proactive in their recovery. Realistic expectations, such as gradual improvement rather than immediate perfect vision, are important for satisfaction. Support from family and caregivers plays a significant role in recovery. Long-term eye protection and regular check-ups help patients maintain the benefits of the transplant for years.
Frequently Asked Questions
How long does a corneal transplant last? Most corneal grafts last 10 to 20 years, though some may last a lifetime.
Is corneal transplant surgery painful? Patients typically experience minimal discomfort, managed with medication or eye drops.
Can both eyes undergo transplant at the same time? Usually, only one eye is treated at a time to allow proper healing and reduce risk.
What is the waiting time for a donor cornea? Waiting periods vary depending on availability and can range from weeks to several months.
Are there alternatives to corneal transplant? Some cases may be managed with corneal cross-linking, specialized contact lenses, or artificial corneas.
Takeaway
Corneal transplant surgery offers a transformative solution for patients with severe corneal damage or disease. Modern techniques, better donor tissue preservation, and proper post-operative care make the procedure highly effective and safe. Patients who prepare well, follow medical instructions, and attend follow-up appointments can enjoy long-lasting improvements in vision and quality of life. Understanding the process, risks, and recovery expectations empowers patients to make informed decisions. Corneal transplantation is not merely surgery; it is a pathway to clearer, healthier vision and a brighter, more confident future.